Research & Reports
MHPA’s research demonstrates the state and value of Medicaid managed care to help inform policy, deepen understanding of performance, and drive quality.
April 2026 -
A Snapshot of Medicaid Managed Care
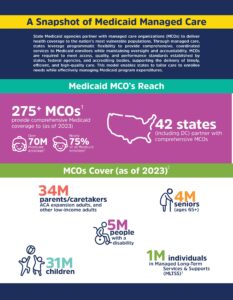
Medicaid managed care organizations (MCOs) partner with states to improve access to primary, preventive, and specialty services for the nation’s most vulnerable populations. The managed care model provides flexibility to address the local, diverse, and complex needs of Medicaid enrollees and improve health outcomes.
As of 2023, over 275 MCOs operate in 42 states and D.C., serving nearly 70 million Medicaid enrollees, which represents approximately 75% of all Medicaid beneficiaries.
VIEW THE RESEARCH BRIEF
October 2025 -
States are Increasingly Enrolling Seniors, People with Disabilities in Medicaid Managed Care
 Historically, state Medicaid programs primarily enrolled low-income children and adults in comprehensive managed care (CMC) while keeping higher-risk populations like seniors and people with disabilities in fee for service. More recently, this trend has changed as states increasingly transition seniors and people with disabilities into CMC to improve consumer choice, service coordination, quality of care, and budget predictability.
Historically, state Medicaid programs primarily enrolled low-income children and adults in comprehensive managed care (CMC) while keeping higher-risk populations like seniors and people with disabilities in fee for service. More recently, this trend has changed as states increasingly transition seniors and people with disabilities into CMC to improve consumer choice, service coordination, quality of care, and budget predictability.
This research brief looks at states’ growing confidence in CMC for Medicaid enrollees qualifying based on age (65+) or disability. The analysis uses T-MSIS enrollment data from 2019-2023 for enrollees receiving full or comprehensive benefits, excluding limited benefit enrollees (e.g., partial-benefit dual eligible enrollees).
VIEW THE RESEARCH BRIEF
July 2025 -
How Medicaid Managed Care Plans Improve Health Outcomes with Quality Improvement Projects
Medicaid Managed Care Plans (MCPs) improve health outcomes by partnering with state Medicaid agencies through Quality Improvement Projects (QIPs). These federally required, multi-year projects test innovative strategies to address priority health issues such as behavioral health, chronic conditions, primary care access, and maternal health. QIPs involve rigorous oversight via independent External Quality Reviews (EQR) to ensure evidence-based methods and data accuracy, with findings used to enhance state Medicaid programs and share best practices.
In 2023-2024, over 1,200 QIPs were independently reviewed across 41 states, focusing on clinical and non-clinical areas including dental care, long-term supports, and enrollee experience. MCPs leverage their expertise in care coordination to implement and refine interventions, driving sustained improvements beyond traditional fee-for-service models.
Overall, QIPs are essential for advancing Medicaid quality, accountability, and health parity by fostering collaboration, innovation, and continuous improvement in managed care settings.
VIEW THE RESEARCH BRIEF
April 2025 -
A Snapshot of Medicaid Managed Care
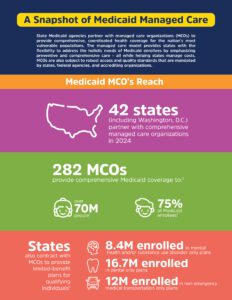
Medicaid managed care organizations (MCOs) partner with states to improve access to primary, preventive, and specialty services for the nation’s most vulnerable populations. The managed care model provides flexibility to address the local, diverse, and complex needs of Medicaid enrollees and improve health outcomes.
As state Medicaid agencies complete post-pandemic eligibility requirements, MCOs continue to play an important role in meeting the health care needs of Medicaid enrollees.
VIEW THE RESEARCH BRIEF
October 2024 -
The Waiver Effect:
An Exploratory Analysis of Medicaid Enrollment Trends in the Presence of Waivers
New research from MHPA reveals that Medicaid Managed Care Organization (MCO)-specific waivers significantly impact enrollment during the unwinding of continuous enrollment. Our analysis of a full year of data shows that states utilizing two waivers experienced the lowest decline in net Medicaid enrollment (11.9% loss) compared to states with zero waivers (15.8% loss).
VIEW THE RESEARCH BRIEF
July 2024 -
 Snapshot of Medicaid with Managed Care - UPDATED
Snapshot of Medicaid with Managed Care - UPDATED
Medicaid managed care organizations (MCOs) partner with states to improve access to primary, preventive, and specialty services for the nation’s most vulnerable populations. The managed care model provides flexibility to address the local, diverse, and complex needs of Medicaid enrollees and improve health outcomes.
As state Medicaid agencies complete post-pandemic eligibility requirements, MCOs continue to play an important role in meeting the health care needs of Medicaid enrollees.
VIEW THE INFOGRAPHIC
January 2024 -
 State of Medicaid Managed Care: A Closer Look at Managed Long-Term Services and Supports
State of Medicaid Managed Care: A Closer Look at Managed Long-Term Services and Supports
To better understand Managed Long-Term Services and Supports (MLTSS) programs, which vary widely in the populations and benefits included under managed care, Sellers Dorsey partnered with MHPA, the Association for Community Affiliated Plans (ACAP), and the National MLTSS Health Plan Association to release "The State of Medicaid Managed Care: A Closer Look at MLTSS." The report features a:
-
Breakdown of key program features of states at various points in the development of MLTSS programs.
-
Survey of states currently operating an MLTSS program on program priorities, dual eligible integration, and more.
-
In-depth look at states' experiences with MLTSS programs including the PHE, Dual Eligibles, Workforce Challenges, and more.



 On the Ground Enrollment: Results from a National Survey of Medicaid MCO Experiences During Redetermination
On the Ground Enrollment: Results from a National Survey of Medicaid MCO Experiences During Redetermination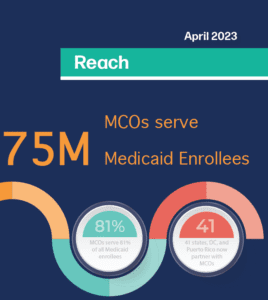 April 2023 -
April 2023 -